-
What is Obstructive Sleep Apnea (OSA)?
Obstructive Sleep Apnea occurs when the throat completely or partially collapses causing interrupted sleep. Snoring occurs when the throat is partially closed and the air passing through causes the throat to vibrate. Apnea is a greek word meaning “no breath”. When you sleep and experience a complete collapse of the upper airway caused by relaxation of the muscles controlling the soft palate and tongue you have an apnea or a total cessation of air flow in the throat.
When you sleep and experience a partial collapse of the upper airway you have a hypopnea causing upper airway tissue vibration also known as snoring.
OSA is classified as being mild, moderate, or severe based upon the number of apneas or hypopneas per hour of sleep. 5 to 14 per hour is considered mild, 15-30 is considered moderate and 30 or more per hour is considered severe.

Closed Airway During an Apnea
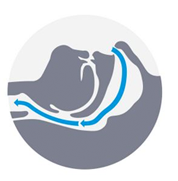
Normal Open Airway
-
What are Common Signs & Symptoms Of OSA?
- Irregular Breathing during Sleep
- Nighttime Gasping, Choking or Coughing
- Frequent Nighttime Urination
- Morning Headaches
- Disruption of bed partner’s sleep
- Excessive Daytime Sleepiness
- Dry Mouth
- Drooling
- Gastroesophageal Reflux
- Depression
- Lack of Energy
-
What are Common Conditions Associated With OSA?
- Approximately 76% of congestive heart failure patients have OSA
- 49% of atrial fibrillation patients have OSA
- Anywhere from 30 to 83% of patients with hypertension have OSA
- 48% of type 2 diabetes sufferers have OSA which may have a causal role in the development of type 2 diabetes
- 86% of obese type 2 diabetes patients have OSA
- 65% of stroke patients have OSA. Moderate to severe sleep apnea triples stroke risk in men
-
If I snore or snort, does this mean I have OSA?
While snoring or snorting during the night can indicate the presence of OSA, a diagnostic sleep study is required to confirm the diagnosis. -
At what age can you develop OSA?
OSA can happen to anyone of any gender of any age. Small infants can have narrow airways which can cause snoring and sleep apnea. A diagnostic sleep study may be required by some insurance providers prior to have tonsils and/or adenoids removed. -
Can fit and thin people get OSA?
OSA does not discriminate, it can occur in anyone of any size or shape. While having some excess weight may increase your chances of developing OSA, body type and weight are not the only determining factors. If you suspect you may have OSA, please discuss this with your primary physician. -
What is a Polysomnogram (Sleep Study)?
A polysomnogram is a study that measures the quality of your sleep. A typical polysomnogram includes the following measures:
- Brain waves (electrodes placed on the scalp)
- Eye movement (electrodes placed on the face, by the eyes)
- Chin muscle tone (electrodes placed on or near the chin)
- Heart rate (electrodes placed on the chest)
- Leg movements (electrodes placed on the legs)
- Breathing (breathing sensor placed near the nose and mouth)
- Breathing effort (two small elastic belts placed around chest and abdomen)
- Oxygen level (small sensor attached to the finger)
- Audio and video recording
-
Why is it necessary to record the above functions?
During sleep, the body functions differently than while awake. Disturbed sleep, such as irregular breathing or lack of sleep consolidation, can interfere with daytime activities, cause daytime sleepiness, and cause serious health problems. -
How can I sleep with all of the electrodes?
Most people sleep reasonably well. The technicians administering your study are looking to obtain a sample of your sleep pattern. The body sensors are applied so that you can move during sleep and change positions during the night. The sleep rooms are set up as comfortable bedrooms, and staff makes the environment as restful as possible. -
Will the sensors hurt?
No. This is a painless and non-invasive (no needles) testing procedure. Paste is applied to your skin and scalp to keep the electrodes in place, but it is easily removed with soap and warm water. -
What is a Multiple Sleep Latency Test (MSLT)?
Some people also participate in daytime testing. This test consists of a series of 20-minute naps. Sensors and electrodes are used to record information similar to the polysomnogram test. 20-minute naps are taken every two hours throughout the day. -
Is the study covered by my Insurance?
Sleep studies are covered under most medical insurance plans, although deductibles and percentages of coverage vary. Details regarding coverage should be directed to your insurance company. -
What is AHI? How is it calculated?
Apnea Hypopnea Index is the number of apneas plus the number of hypopneas per hour while sleeping. This number is used to determine the severity of a patient’s obstructive sleep apnea.
To determine your AHI add the total number of apnea and hypopnea events, divide by the total number of minutes of actual sleep time, then multiply that number by 60.
Example:
Apnea + Hypopnea multiplied by 60, then divided by actual total sleep time
100 Apneas, 100 Hypopnea (200 Total Events)
360 Minutes Actual Sleep time (6 hours x 60 minutes)
Multiply 200 x 60 =12000 / 360 = 33 AHI (Severe OSA)
The Severity of OSAHS as defined by the American Academy of Sleep Medicine Task Force (1999) is:<5 per hour = Normal
5 - 15 per hour = Mild
15 - 30 per hour = Moderate
> 30 per hour = Severe -
How Sleep Apnea is Treated?
- Continuous Positive Airway Pressure (CPAP)
Continuous positive airway pressure (CPAP) is the frontline treatment for obstructive sleep apnea. CPAP keeps your airway open during the night by gently providing a constant stream of air through a mask you wear while you sleep. This will eliminate the breathing pauses caused by OSA, so you will no longer snore or make choking noises in your sleep. You will be able to sleep through the night without your body waking up from lack of oxygen.
When you use CPAP, you will feel more alert during the daytime. Your mood will improve and you will have a better memory. CPAP prevents or even reverses serious health problems associated with sleep apnea such as heart disease and stroke. Your partner may even sleep better because you will stop snoring.
CPAP comes with a machine, a hose for air and a mask. Most machines are small – about the size of a tissue box – lightweight and relatively quiet. You can keep the CPAP machine on your nightstand or at the side of your bed.
Research shows treatment of OSA using CPAP therapy improves daytime blood pressure, heart rate and reduces blood glucose levels.
- Oral Appliance Therapy
Oral Appliance Therapy involves the selection, fitting and use of a specially designed oral appliance that maintains an open, unobstructed airway when worn during sleep. Oral appliances reposition and maintain the lower jaw in a protruded position during sleep. This opens the airway by indirectly pulling the tongue and soft tissue behind the tongue forward.
- Weight Loss
Weight changes can significantly affect the severity of sleep apnea, perhaps even leading to a reassessment of the degree of OSA and CPAP requirements.
- Avoiding Certain Medications
Benzodiazepines, narcotics, and alcohol reduce upper airway muscle tone and should be avoided. No medications are associated with improvement of OSA.
- Positional Therapy
Sometimes sleep apnea is much worse when lying on your back compared to sleeping on your side. In such instances the use of a “bumper belt” which forces you to sleep on your side may be a sufficient remedy for OSA.
- Surgical Interventions
Some patients with sleep disordered breathing may be candidates for a surgical intervention. A surgeon board certified in sleep medicine should be contacted to evaluate anyone interested in exploring a surgical option.
- Continuous Positive Airway Pressure (CPAP)
Important! If you are suffering from any of these symptoms, see a doctor right away and do not try to diagnose yourself. There are other more serious conditions which share the same symptoms.
